The role of monocytes in the progression of sepsis
The increasing global burden of sepsis in healthcare calls for better diagnostic tests that allow earlier detection of sepsis and infections that could lead to sepsis. The major problem for patients at risk for sepsis is an immunological imbalance. Cells of the innate immune system, such as monocytes and neutrophils, are the first-line of defence against infections. In the presence of sepsis, these cells produce a flood of inflammatory cytokines, causing widespread inflammation that can lead to death. Monocytes perform multiple immunological functions, and play a role in the development of sepsis-induced inflammation and immunosuppression. Monocyte subpopulations with different functions and morphologies vary in number over the course of the inflammatory response. The monocyte distribution width (MDW) is a novel cellular marker of monocyte anisocytosis that can add significant value to the white blood cell (WBC) count and help detect sepsis in patients entering the emergency department (ED).
by Elena A. Sukhacheva
Sepsis epidemiology and definitions
Sepsis is a major healthcare burden and, despite progress in diagnostic and treatment options, mortality from sepsis remains unacceptably high. The number of septic patients in the U.S., UK and EU is increasing [1–4]. Clearly, there is an unmet need for better diagnostic tests that can provide both the early detection of sepsis and the detection of severe infections that may progress to sepsis, if not diagnosed early enough. Global increases in sepsis frequency may be related to the aging population, as the incidence of sepsis is disproportionately increased in elderly adults, and age is an independent predictor of mortality [5]. Furthermore, immunosuppressive drugs, which are increasingly being used for diverse conditions, may result in more severe infections and increased sepsis frequency [6].
The definition of sepsis has recently been changed from the previous Sepsis-2 definition of a systemic inflammatory response (SIRS) in the presence of an infection [7], to the current Sepsis-3 definition of a life-threatening organ dysfunction caused by a dysregulated host response to infection [8]. The new Sepsis-3 definition reflects newfound understanding that the immune response in sepsis is more complex than previously thought, comprising both pro- and anti-inflammatory mechanisms.
Immune response in sepsis
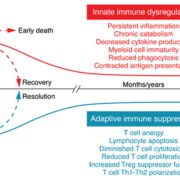
It is now clear that the major problem for patients with sepsis, or at high risk of developing sepsis, is immunological imbalance, and dysregulation of the mechanisms of innate and adaptive immunity. Sepsis occurs when the immune system begins, in one way or another, to lose the battle against severe infection. After sepsis onset, the production of pro-inflammatory cytokines (IL-1β, IL-6, and tumour necrosis factor [TNFα]) by the cells of the innate immune system (neutrophils and monocytes) may result in a “cytokine storm” that produces overwhelming inflammation, which can lead to blood pressure collapse, coagulation abnormalities and, ultimately, organ failure and death. In the later stages of disease, patients who survive the cytokine storm may die from sepsis-related immunosuppression and an inability of the immune system to combat infection efficiently [9]. Inflammatory and immunosuppressive processes may overlap in sepsis [10,11], further complicating the biology of this fatal condition whose mechanisms are still poorly understood by scientists. Figure 1 shows the current understanding of immune imbalance in sepsis [12]. While all immune cells are involved in the immune response in sepsis [13–16] (Figure 2), this document is mainly focused on changes in monocytes, with other cell populations discussed only briefly.
Under normal conditions, neutrophils usually stay in the circulation for only a few hours and undergo apoptosis within 24 hours of release from the bone marrow. In sepsis, the delay in neutrophil apoptosis [17,18], combined with the increased neutrophil production in the bone marrow, results in neutrophilia. The function of these neutrophils, however, is impaired [19], with decreased chemotactic activity [20,21], decreased antibacterial function and increased production of anti-inflammatory cytokine interleukin 10 (IL-10) [22].
Sepsis also has a profound effect on all the main lymphocyte subpopulations [14]: CD4+ T-cells, CD8+ T-cells and B-cells undergo increased apoptosis; T-regulatory cells are more resistant to sepsis-induced apoptosis, leading to an increased proportion of T-regulatory cells and an immunosupressive phenotype. T-helper cell polarization from a pro-inflammatory Th1 phenotype towards an anti-inflammatory Th2 phenotype also contributes to increased immunosuppression in sepsis.
Monocytes also undergo multiple changes in sepsis, but before discussing these phenomena, it is important to discuss some basic information about the biology and classification of monocytes.
Monocytes’ biology and classification
Monocytes are cells of the innate immune system, the body’s first-line of defence against infection. Other cells of this system include neutrophils, basophils, eosinophils, mast cells, as well as certain types of lymphocytes such as γδ-T-cells and natural killer cells. The innate immune response develops during the first hours and days after pathogen invasion, and the majority of pathogens entering the human body usually are inactivated by this response and do not require adaptive mechanisms with lymphocyte involvement.
Myeloid precursors in the bone marrow differentiate into promonocytes and then into mature monocytes that enter the peripheral blood. These monocytes stay in the circulation for one to three days, after which they migrate into tissues and organs, where they turn into macrophages and dendritic cells. Morphologically, monocytes are large cells measuring 10 to 18 µm in diameter, with convoluted nuclei and azurophilic granules in their cytoplasm.
Monocytes and dendritic cells perform multiple immunological functions that include phagocytosis, antigen presentation and cytokine production. The function of these cells is regulated by a number of cell surface receptors:
- CD14, the receptor for complexes of bacterial lipopolysaccharides and human serum proteins
- Receptors such as CD163 that scavenge membrane fragments and other components of damaged cells
- Multiple receptors for the Fc regions of IgG: CD64 (FcγR1, high-affinity receptor), CD32 (FcγR2, medium-affinity receptor) and CD16 (FcγR3, present only on subpopulations of so-called pro-inflammatory monocytes)
- Other receptors necessary for interaction with lymphocytes and receptors for cytokines
Three subpopulations of monocytes have been characterized in peripheral blood [23–25]. Classical monocytes make up the main monocyte population. Expressing high level CD14 and no CD16 (CD14++CD16-), they represent 80–90% of monocytes in peripheral blood. “Intermediate” monocytes expressing CD16 (CD14++CD16+) are normally found at low numbers, but increase with cytokine stimulation and inflammation. Nonclassical monocytes display decreased expression of CD14 and increased expression of CD16 (CD14+CD16++), and comprise 9%+/-5% of all monocytes, with an average count in healthy donors of approximately 45+/-22 cells/µL [26].
In the literature, nonclassical monocytes are sometimes referred to as inflammatory or pro-inflammatory monocytes; however, published recommendations for the nomenclature of monocytes and dendritic cells in the blood clearly advocate avoiding functional terminology, “because this leads to confusion as the label ‘inflammatory’ has been used for different subpopulations in humans and mice [24].” Also, “these terms may prematurely ascribe functional attributes to cells based on ex vivo studies while they largely remain to be functionally characterized in vivo [24].” Subsets of nonclassical monocytes are expanded dramatically in several pathological conditions including sepsis [26–28], HIV-1 infection [29–33], diabetes [34–35], tuberculosis [36] and other disease states [37].
The recent detailed analysis performed by Mukherjee et al. [28] revealed the functions of monocyte subsets as follows: classical monocytes are phagocytic with no inflammatory attributes, nonclassical subtypes display inflammatory characteristics on activation and display properties for antigen presentation, and intermediate subtypes appear to have both phagocytic and inflammatory functions [28]. In 2017, research based on single-cell RNA sequencing discovered even more subtypes, describing six subpopulations of dendritic cells and four monocyte subpopulations [39]. This classification was based solely on transcriptional activity, and further studies will be needed to understand function and describe the phenotype of all cell subpopulations. Nonetheless, it is clear that morphologically similar cells that we call monocytes may actually have very different functions in human immunity.
Monocytes in sepsis
Monocytes, as cells of first-line defence against infection, are involved in the immune response from very early stages. Abundant literature exists on monocytes and the changes they undergo in sepsis.
A recent study on the dynamics of monocyte subpopulations in peripheral blood at the onset of infection has demonstrated a decrease in the number of peripheral blood monocytes during the early stages of lipopolysaccharide (LPS)-induced acute inflammation in humans. This loss may be due to the migration of monocytes from the blood into tissues, where they differentiate into macrophages and dendritic cells, or it may reflect an increase in monocytes residing in the marginal pool or rolling on the vessel walls [40]. For all three subpopulations of monocytes, the number of cells was decreased at one to two hours after LPS injection. This decrease was followed by a return to the baseline count, but with differences in timing for the three monocyte subsets. This difference in timing means that the early stages of infection, before the appearance of any clinical symptoms, are characterized by differences in the proportions of monocyte subpopulations relative to baseline pre-infection proportions.
Functional changes in monocytes and, in parallel, changes in their cellular morphology, have been demonstrated in the past for a human THP-1 monocytic cell line infected with viable C. pneumonia bacteria [41]. The differentiation of infected cells into macrophages was accompanied by a change to an ameboidor diffused morphology as assessed by microscopy after Giemsa staining.
Multiple studies have demonstrated the importance of HLA-DR expression on monocytes as a prognostic marker in septic patients. A decreased level of HLA-DR expression on monocytes has been found to be a negative prognostic indicator [42–44] and may be used to evaluate the functional activity of the immune system [45,46]. Decreased HLA-DR, as a marker of monocyte anergy, correlates with decreased antigen presentation capacity and decreased pro-inflammatory cytokine release. This has been analyzed mainly by flow cytometry, but, recently, new methods based on real-time PCR have emerged [47,48].
Another monocyte marker, CD16, plays an important role in orchestrating the response of monocytes to Gram-negative sepsis. It has been demonstrated that CD16 on human monocytes is a key regulator of the TRIF-dependent TLR4 signalling pathway, and this pathway is preferentially activated in the CD16+ monocyte subset [49]. Recent publications suggest the variability of monocyte properties in sepsis. Detailed analysis of gene expression in patient monocytes during sepsis and after recovery demonstrated plasticity of monocytes in the course of disease [50]. The significant up-regulation of pro-inflammatory cytokines (IL-1b, IL-6) and chemokines (CCL3 and CCL5) has been demonstrated in sepsis monocytes compared to monocytes after recovery. Transcriptional factor NF-kB, a central transcriptional regulator of the inflammatory response, was also activated in sepsis monocytes, supporting their involvement in severe inflammation. At the same time, anti-inflammatory cytokine IL-10 was found to be up-regulated in sepsis monocytes. These studies once again highlight the diversity of monocytes’ function in sepsis pathogenesis, and their key role in disease progression, with the possible polarization from a pro-inflammatory state to an immunosuppressive state.
More recently, Crouser et al. demonstrated that the morphological variability that occurs during monocyte activation in the early inflammatory response can be captured by measuring the monocyte distribution width (MDW), an indicator of monocyte anisocytosis. Investigators showed that MDW could be a novel cellular marker that may help detect sepsis early in patients admitted to the emergency department (ED) [51]. Multiple morphometric characteristics of monocytes were obtained using a DxH 800 cellular analysis system, which employs physical measurement of cell volume, conductivity and multiple angles of laser scatter to classify leukocytes into five sub-populations and detect the presence of abnormal cells. This study showed that anisocytosis of circulating monocytes provides significant added value to WBC count for the detection of sepsis in the ED population.
Conclusion
In summary, monocytes are a very heterogeneous population of cells that differ in phenotype, size, nuclear morphology, gene profile and function [52]. In sepsis, this diversity is even more pronounced due to functional changes of monocyte subsets, and is accompanied by a variation in monocyte morphology.
Morphological variability is just the tip of the iceberg of the underlying biological heterogeneity, and may be an important early marker of sepsis or severe infections with a high risk of progressing to sepsis. A recent publication from Crouser [51], together with previous research on sepsis using cellular morphometric parameters gathered using a DxH 800 analyser [53–56], may build the foundation for practical usage of MDW in combination with currently-used sepsis markers (WBC, PCT, CRP, IL-6) for early sepsis screening and diagnosis, leading to early initiation of appropriate therapy.
References
1. Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR. “Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care.” Crit Care Med, 2001, vol. 29, no.7, pp. 1303–1310.
2. Brun-Buisson C, Meshaka P, Pinton P, Vallet B. “EPISEPSIS Study Group. EPISEPSIS: a reappraisal of the epidemiology and outcome of severe sepsis in French intensive care units.” Intensive Care Med, 2004, vol. 30, pp. 580–588.
3. van Gestel A, Bakker J, Veraart CP, van Hout BA. “Prevalence and incidence of severe sepsis in Dutch intensive care units.” Crit Care, 2004, vol. 8, pp. R153–62.
4. Harrison DA, Welch CA, Eddleston JM. “The epidemiology of severe sepsis in England, Wales and Northern Ireland, 1996 to 2004: secondary analysis of a high quality clinical database, the ICNARC Case Mix Programme Database.” Crit Care, 2006, vol. 10, p. R42.
5. Martin GSM, Mannino DM, Moss M. “The effect of age on the development and outcome of adult sepsis.” Crit Care Med, 2006, vol. 34, no.1, pp. 15–21.
6. Gea-Banacloche JC, Opal SM, Jorgensen J, Carcillo JA, Sepkowitz KA, Cordonnier C. “Sepsis associated with immunosuppressive medications: an evidence-based review.” Crit Care Med, 2004, vol. 32, no. 11 (suppl.), pp. S578–90.
7. Bone RC, et al. “Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine.” Chest, 1992, vol. 101, pp.1644–55.
8. Singer M, et al. “The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3).” JAMA, 2016, vol. 315, no. 8, pp.801–810.
9. Hotchkiss RS, Monneret G, Payen D. “Immunosuppression in sepsis: a novel understanding of the disorder and a new therapeutic approach.” Lancet Infect Di,. 2013, vol. 13, no. 3, pp. 260–268.
10. Adib-Conquy M, Cavaillon JM. “Compensatory anti-inflammatory response syndrome.” Thromb Haemost, 2009, vol. 101, pp. 36–47.
11. Gomez HG, Gonzalez SM, Londoño JM, Hoyos NA, Niño CD, Leon AL, Velilla PA, Rugeles MT, Jaimes FA. “Immunological characterization of compensatory anti-inflammatory response syndrome in patients with severe sepsis: a longitudinal study.” Crit Care Med, 2014, vol. 42, no 4, pp.771–80.
12. Delano MJ, Ward PA. “Sepsis-induced immune dysfunction: can immune therapies reduce mortality?” J Clin Invest, 2016, vol. 126, no. 1, pp. 23–31.
13. Bosmann M. and Ward PA. “The inflammatory response in sepsis.” Trends Immunol, 2013, vol. 34, no. 3, pp. 129–136.
14. Hotchkiss RS, Monneret G, Payen D. “Sepsis-induced immunosuppression: from cellular dysfunctions to immunotherapy.” Nat Rev Immunol, 2013, vol. 13, no. 12, pp. 862–874.
15. Van der Poll T, van de Veerdonk FL, Scicluna BP, Netea MG. “The immunopathology of sepsis and potential therapeutic targets.” Nat Rev Immunol, 2017, vol. 17, pp. 407–420.
16. Stearns-Kurosawa DJ, Osuchowski MF, Valentine C, Kurosawa S, Remick DG. “The pathogenesis of sepsis.” Annu Rev Pathol, 2011, vol. 6, pp. 19–48.
17. Paunel-Görgülü A, Kirichevska T, Lögters T, Windolf J, Flohé S. “Molecular mechanisms underlying delayed apoptosis in neutrophils from multiple trauma patients with and without sepsis.” Mol Med, 2012 vol. 18, pp. 325–335.
18. Tamayo E, Gómez E, Bustamante J, Gómez-Herreras JI, Fonteriz R, Bobillo F, Bermejo-Martín JF, Castrodeza J, Heredia M, Fierro I, Álvarez FJJ “Evolution of neutrophil apoptosis in septic shock survivors and nonsurvivors.” Crit Care, 2012 vol. 27, no. 4, pp. 415.e1–11.
19. Alves-Filho JC, Spiller F, Cunha FQ. “Neutrophil paralysis in sepsis.” Shock, 2010, vol. 34, Suppl 1, pp. 15–21.
20. Kovach MA, Standiford TJ. “The function of neutrophils in sepsis.” Curr Opin Infect Dis. 2012, vol. 25, pp. 321–327.
21. Cummings CJ, et al. “Expression and function of the chemokine receptors CXCR1 and CXCR2 in sepsis.” J Immunol, 1999, vol. 162, pp. 2341–6.
22. Kasten KR, Muenzer JT, Caldwell CC. “Neutrophils are significant producers of IL-10 during sepsis.” Biochem Biophys Res Commun, 2010, vol. 393, pp. 28–31.
23. B Passlick, D Flieger, HW Ziegler-Heitbrock. “Identification and characterization of a novel monocyte subpopulation in human peripheral blood.” Blood, 1989, vol. 74, pp. 2527–2534.
24. Ziegler-Heitbrock L, Ancuta P, Crowe S, Dalod M, Grau V, Hart DN, Leenen PJ, Liu YJ, MacPherson G, Randolph GJ, Scherberich J, Schmitz J, Shortman K, Sozzani S, Strobl H, Zembala M, Austyn JM, Lutz MB. “Nomenclature of monocytes and dendritic cells in blood.” Blood, 2010 vol. 116, no. 16, e74–80.
25. Guilliams M, Ginhoux F, Jakubzick C, Naik SH, Onai N, Schraml BU, Segura E, Tussiwand R, Yona S. “Dendritic cells, monocytes and macrophages: a unified nomenclature based on ontogeny.” Nat Rev Immunol, 2014, vol. 14, no. 8, pp. 571–578.
26. Fingerle G, Pforte A, Passlick B, Blumenstein M, Strobel M, Ziegler-Heitbrock HWL. “The novel subset of CD14+/CD16+ blood monocytes is expanded in sepsis patients.” Blood, 1993, vol. 82, pp. 3170–3176.
27. Skrzeczynska, J, Kobylarz K, Hartwich Z,Zembala M, Pryjma J. “CD14+ CD16+ monocytes in the course of sepsis in neonates and small children: monitoring and functional studies.” Scandinavian J Immun, 2002, vol. 55, no. 6, pp. 629–638.
28. Mukherjee R, Barman PK, Thatoi PK, Tripathy R, Das BK, Ravindran B. “Non-classical monocytes display inflammatory features: validation in sepsis and systemic lupus erythematous.” Scientific Reports, 2015, vol. 5:13886 | DOI: 10.1038/srep13886.
29. Funderburg NT, Zidar DA, Shive C, Lioi A, Mudd J, Musselwhite LW, Simon DI, Costa MA, Rodriguez B, Sieg SF, Lederman MM. “Shared monocyte subset phenotypes in HIV-1 infection and in uninfected subjects with acute coronary syndrome.” Blood, 2012, vol. 120, no. 23, pp. 599–608.
30. Chen P, Su B, Zhang T, Zhu X, Xia W, Fu Y, Zhao G, Xia H, Dai L, Sun L, Liu L, Wu H. “Perturbations of monocyte subsets and their association with T helper cell differentiation in acute and chronic HIV-1¬infected patients.” Front Immunol, 2017, vol. 8, p. 272.
31. Williams DW, Calderon TM, Lopez L, Carvallo-Torres L, Gaskill PJ, Eugenin EA, Morgello S, Berman JW. “Mechanisms of HIV entry into the CNS: increased sensitivity of HIV infected CD14+CD16+ monocytes to CCL2 and key roles of CCR2, JAM-A, and ALCAM in diapedesis.” PLoS One, 2013, vol. 8, no 7:e69270.
32. Ansari AW, Meyer-Olson D, Schmidt RE. “Selective expansion of pro-inflammatory chemokine CCL2¬loaded CD14+CD16+ monocytes subset in HIV-infected therapy naïve individuals.” J Clin Immunol, 2013, vol. 33, no. 1, pp. 302–306.
33. Dutertre CA, Amraoui S, DeRosa A, Jourdain JP, Vimeux L, Goguet M, Degrelle S, Feuillet V, Liovat AS, Müller-Trutwin M, Decroix N, Deveau C, Meyer L, Goujard C, Loulergue P, Launay O, Richard Y, Hosmalin A. “Pivotal role of M-DC8 monocytes from viremic HIV-infected patients in TNFα overproduction in response to microbial products.” Blood, 2012, vol. 120, no. 11, pp. 2259–68.
34. Min D, Brooks B, Wong J, Salomon R, Bao W, Harrisberg B, Twigg SM, Yue DK, McLennan SV. “Alterations in monocyte CD16 in association with diabetes complications.” Mediators Inflamm, 2012; vol. 2012, Article ID 649083.
35. Ryba-Stanisławowska M, Myśliwska J, Juhas U, Myśliwiec M. “Elevated levels of peripheral blood CD14(bright) CD16+ and CD14(dim) CD16+ monocytes may contribute to the development of retinopathy in patients with juvenile onset type 1 diabetes.” APMIS, 2015, vol. 123, no. 9, pp. 793–9.
36. Lugo-Villarino G, Neyrolles O. “Dressed not to kill: CD16+ monocytes impair immune defence against tuberculosis.” Eur J Immunol, 2013, vol. 43, no. 2, pp. 327–30.
37. Fingerle-Rowson G, Auers J, Kreuzer E, Fraunberger P, Blumenstein M, Ziegler-Heitbrock LH. “Expansion of CD14+CD16+ monocytes in critically ill cardiac surgery patients.” Inflammation, 1998, vol. 22, pp. 367–79.
38. Lee J, Tam H, Adler L, Ilstad-Minnihan A, Macaubas C, Mellins ED. “The MHC class II antigen presentation pathway in human monocytes differs by subset and is regulated by cytokines.” PLoS One, 2017, vol. 12, no. 8, e0183594.
39. Villani AC, Satija R, Reynolds G, Sarkizova S, Shekhar K, Fletcher J, Griesbeck M, Butler A, Zheng S, Lazo S, Jardine L, Dixon D, Stephenson E, Nilsson E, Grundberg I, McDonald D, Filby A, Li W, De Jager PL, Rozenblatt-Rosen O, Lane AA, Haniffa M, Regev A, Hacohen N. “Single-cell RNA-seq reveals new types of human blood dendritic cells, monocytes, and progenitors.” Science, 2017, vol. 356, issue 6335, eaah4573.
40. Tak T, van Groenendael R, Pickkers P, Koenderman L. “Monocyte subsets are differentially lost from the circulation during acute inflammation induced by human experimental endotoxemia.” J Innate Immun, 2017, vol. 12, no. 9, pp. 464–74.
41. Yamaguchi Y, Haranaga S, Widen R, Friedman H, Yamamoto Y. “Chlamydia pneumoniae infection induces differentiation of monocytes into macrophages.” Infection and Immunity, 2002, vol. 70, pp. 2392–8.
42. Strohmeyer JC, Blume C, Meisel C, Doecke WD, Hummel M, Hoeflich C, Thiele K, Unbehaun A, Hetzer R, Volk HD. “Standardized immune monitoring for the prediction of infections after cardiopulmonary bypass surgery in risk patients.” Cytometry B Clin Cytom, 2003, vol. 53, no. 1, pp. 54–62.
43. Genel F, Atlihan F, Ozsu E, Ozbek E. “Monocyte HLA-DR expression as predictor of poor outcome in neonates with late onset neonatal sepsis.” J Infect, 2010, vol. 60, no. 3, pp. 224–228.
44. Satoh A, Miura T, Satoh K, Masamune A, Yamagiwa T, Sakai Y, Shibuya K, Takeda K, Kaku M, Shimosegawa T. “Human leukocyte antigen-DR expression on peripheral monocytes as a predictive marker of sepsis during acute pancreatitis.” Pancreas, 2002, vol. 25, no. 3, pp. 245–250.
45. Volk HD, Reinke P, Döcke WD. “Immunological monitoring of the inflammatory process: Which variables? When to assess?” Eur J Surg Suppl, 1999, vol. 584, pp. 70–72.
46. Winkler MS, Rissiek A, Priefler M, Schwedhelm E, Robbe L, Bauer A, Zahrte C, Zoellner C, Kluge S, Nierhaus A. “Human leucocyte antigen (HLA-DR) gene expression is reduced in sepsis and correlates with impaired TNFα response: A diagnostic tool for immunosuppression?” PLoS One, 2017, vol. 12, no. 8, p. e0182427.
47. Cajander S, Bäckman A, Tina E, Strålin K, Söderquist B, Källman J. “Preliminary results in quantitation of HLA-DRA by real-time PCR: a promising approach to identify immunosuppression in sepsis.” Crit Care, 2013, vol. 17, p. R223.
48. Monneret G, Venet F. “Monocyte HLA-DR in sepsis: shall we stop following the flow?” Crit Care, 2014, vol. 18:102.
49. Shalova IN, Kajiji T, Lim JY, Gomez-Pina V, Fernandez-Ruiz I, Arnalich F et al. “CD16 regulates TRIF-dependent TLR4 response in human monocytes and their subsets.” J Immunol, 2012, vol. 188, pp. 3,584–3,593.
50. Shalova IN, Lim JY, Chittezhath M, Zinkernagel AS, Beasley F, Hernandez-Jimenez E, Toledano V, Cubillos-Zapata C, Rapisarda A, Chen J, Duan K, Yang H, Poidinger M, Melillo G, Nizet V, Arnalich F, Lopez-Collazo E, Biswas SK. “Human monocytes undergo functional re-programming during sepsis mediated by hypoxia-inducible factor-1a.” Immunity, 2015, vol. 42, pp. 484–498.
51. Crouser ED, Parrillo JE, Seymour C, Angus DC, Bicking K, Tejidor L, Magari R, Careaga D, Williams J, Closser DR, Samoszuk M, Herren L, Robart E, Chaves F. “Improved early detection of sepsis in the ED with a novel monocyte distribution width biomarker.” Chest, 2017 vol. 152, no. 3, pp. 518–526.
52. Yona S, Jung S. “Monocytes: subsets, origins, fates and functions” Curr Opinion in Hematology, 2010, vol. 17, pp.53–59.
53. Abiramalatha T, Santhanam S, Mammen JJ, Rebekah G, Shabeer MP, Choudhury J, Nair SC. “Utility of neutrophil volume conductivity scatter (VCS) parameter changes as sepsis screen in neonates.” J Perinatol, 2016, vol. 36, no. 9, pp. 733–738.
54. Lee A-J, Kim S-G. “Mean cell volumes of neutrophils and monocytes are promising markers of sepsis in elderly patients.” Blood Research, 2013, vol. 48, no. 3, pp. 193–197.
55. Park D-H, Park K, Park J, Park H-H, Chae H, Lim J, Oh E-J, Kim Y, Park YJ, Han K. “Screening of sepsis using leukocyte cell population data from the Coulter automatic blood cell analyzer DxH800.” Int Jnl Lab Hem, 2011, vol. 33, pp. 391–399.
56. Dilmoula A, Kassengera Z, Turkan H, Dalcomune D, Sukhachev D, Vincent JL, and Pradier O. “Volume, conductivity and scatter properties of leukocytes (VCS technology) in detecting sepsis in critically ill adult patients.” Blood (ASH Annual Meeting Abstracts), 2011, vol. 118, abstract 4729.
The author
Elena A. Sukhacheva, Ph.D.
Senior Manager,
Global Scientific Affairs, Hematology, Beckman Coulter Diagnostics,
Miami, FL, USA