Apolipoproteins – new perspectives for lipid profiling, but other challenges remain
Atherosclerotic cardiovascular diseases (CVD) are the leading cause of death in the West, and dyslipidemia is considered to be one of their key risk factors. The majority of CVD cases could be prevented by effective management of dyslipidemia. The use of new biomarkers like apolipoproteins as part of extended lipid profiles may be among the most significant new tools for such a task.
Dyslipidemias
Dyslipidemias cover a broad spectrum of lipid abnormalities. Clinicians have so far paid maximum attention to elevated levels of total cholesterol (TC) and low-density lipoprotein-cholesterol (LDL-C). Many other types of dyslipidemias, however, also appear to enhance the risk of CVD.
Lipid metabolism can become imbalanced or disturbed in several ways, resulting in changes to plasma lipoprotein function and thereafter to the development of atherosclerosis. Many patients who have high cardiovascular risk still have unfavourable lipid profiles.
Given the fast-growing interest in lipidology, clinicians have sought ways to apply evidence-based medicine daily in dyslipidemia management. There are several lipid guidelines from professional societies in different parts of the world to diagnose and make assessments of dyslipidemia.
The role of apolipoproteins
In recent years, both Europe and the US have witnessed revisions in CVD guidelines and in the approach to lipid profiling. One major new area of attention is the role of apolipoproteins.
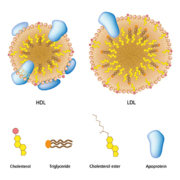
Apolipoproteins serve to bind lipids (fat and cholesterol) to form lipoproteins. Lipids are insoluble in water. However, apolipoproteins have amphiphilic (detergent-like) properties, which make them both fat- and water-soluble. As a result, the lipoprotein particle effectively becomes water-soluble, allowing for the transport of lipids through the lymph and circulatory systems. Apolipoproteins also regulate lipoprotein metabolism.
So far, most efforts have been focused on two apolipoproteins, apolipoprotein B (apo B) and apo A-I.
From a technical viewpoint, there are numerous advantages in determining concentrations of apo B and apo A-I. Robust immunochemical methodologies are possible to attain with conventional assays using appropriate reagents. These methodologies have also been shown to provide required levels of analytical performance. Moreover, apo assays do not require fasting conditions and are not sensitive to moderately high levels of triglycerides (TG).
Apo B
Apo B is the main protein in LDL-C and directly associated with cholesterol uptake. Elevated apo B indicates an increased risk of CVD even when total cholesterol and LDL-C levels are otherwise normal.
In the laboratory, apo B concentration provides a good indicator of the number of particles in plasma of VLDL (very low-density lipoprotein), IDL (intermediate-density lipoprotein) and LDL (low-density lipoprotein).
Apo B has aroused especially high interest given its presence in high concentrations of small dense LDL. The latter is seen to be “an important predictor of cardiovascular events and progression of coronary artery disease (CAD)” and it has been endorsed as an emerging cardiovascular risk factor by the US National Cholesterol Education Program Adult Treatment Panel III in 2007.
Some contradictory evidence indicates need for more study
A host of prospective studies have shown apo B to be equal to LDL-C in risk prediction. Post-hoc analyses of numerous statin trials suggest that apo B may be not only a good biomarker but also a better treatment target than LDL-C.
However, verifying this is likely to take some more years. Apo B is yet to be included in risk calculation algorithms. Meanwhile, data about its utility remains contradictory.
For example, a meta-analysis by the Emerging Risk Factor Collaboration in 2009 indicates that apo B does not provide any benefit beyond non-high-density lipoprotein cholesterol (non-HDL-C) or traditional lipid ratios. A year later, apo B showed no benefit compared to traditional lipid markers in diabetics in the so-called FIELD study (Fenofibrate Intervention and Event Lowering in Diabetes). On the other hand, in 2011, another meta-analysis of LDL-C, non-HDL-C and apo B conducted by Canadian researchers found the apolipoprotein to be a superior marker of CV risk. Indeed, the authors, from the Royal Victoria Hospital at McGill University concluded that apo B would prevent more than one-and-a-half times the number of CV events compared to a non-HDL-C strategy alone.
Apo A-I and HDL
Unlike apo B (and LDL cholesterol), apo A-I is the major protein of HDL and provides a good estimate of HDL concentration. One HDL particle could carry several apo A-I molecules. So far, plasma apo A-I correspondences have been established (with levels of <120 mg/dL for men and <140 mg/dL for women) correlating to ‘low’ HDL-C.
Apo A-I is sometimes tested alongside apo B. The ratio between apo B and apo A-I can be used as an alternative to the total cholesterol/HDL cholesterol ratio or non-HDL-C/HDL-C ratio for indicating risk. However, as with the latter, for diagnosis and treatment, the components of the ratio have to be considered separately.
Other apolipoproteins
Research is also under way into the other apolipoproteins. Indeed, several clinical labs already offer analysis of their concentrations. These include apo A-II, apo C-II and C-III and apo E and have also provoked interest in clinical researchers.
Like apo A-I, apo A-II is also a major constituent of HDL-C, and the distribution of the former in HDL is primarily determined by the rate of production of apo A-II. Apo A-II has an important role in reverse cholesterol transport and lipid metabolism. Its increased production promotes atherosclerosis by decreasing the proportion of anti-atherogenic HDL containing Apo A-I.
Apo C-II is a co-factor for lipoprotein lipase, which breaks down lipoproteins and hydrolyses triglycerides and VLDL for absorption into tissue cells. Low concentrations of apo C-II have been linked with hypertriglyceridemia.
Apo C-III modulates uptake of triglyceride-rich lipoproteins by LDL receptor related proteins through inhibition of lipoprotein lipase. Elevated apo C-III levels are associated with both primary and secondary hypertriglyceridemia.
Apo E is found in IDLs and has several functions. These include transporting triglycerides to the liver and distributing cholesterol between cells. Apo B affects the formation of atherosclerotic lesions by inhibiting platelet aggregation and its deficiency provokes high serum cholesterol and triglyceride levels, leading to premature atherosclerosis.
CVD guidelines and apolipoproteins
In spite of the growing interest in other apolipoproteins, the highest level of interest is on apo B and A-1. Both are covered by recent modifications in certian CVD guidelines.
In 2011, the European Atherosclerosis Society (EAS) and the European Society of Cardiology (ESC) updated several CVD guidelines. Changes included doubling the stratification of cardiovascular risk from two to four categories – “very high”, “high”, “moderate” and “low”, along with the tightening of therapeutic targets for each category.
While acceptable LDL-C levels were reduced significantly across risk groups, two new therapeutic targets were recommended for patients in “very high” and “high” risk categories, especially those with combined dyslipidemia. These consisted of non-HDL cholesterol and apolipoprotein (apo) B levels.
In Europe, updated EAS/ESC guidelines recommend baseline lipid evaluation be made either on the basis of TC (total cholesterol), TG, HDL-C, and LDL-C. These are typically calculated by the so-called Friedewald formula. The new guidelines also propose using “apo B and the apo B/apo A1 ratio,” which it acknowledges are “at least as good risk markers compared with traditional lipid parameters.”
Meanwhile, in the US, professional endocrinology bodies have directly enhanced their focus on dyslipidemia since 2012, when the American Association of Clinical Endocrinologists (AACE) released new clinical practice guidelines (CPG) on the ‘Management of Dyslipidemia and Prevention of Atherosclerosis’.
The AACE’s aim was to update its existing CPGs and to complement the Diabetes Mellitus Comprehensive Care Plan CPG. Nevertheless, the AACE emphasizes that the ‘landmark’ National Cholesterol Education Program (NCEP) guidelines of 1993 continued to serve as the ‘backbone’ of its revised recommendations.
Though the new CPGs from the AACE continue to emphasize the importance of LDL-C reduction and support the measurement of inflammatory markers to stratify risk in certain situations, they nevertheless have several noteworthy features. What makes them unique for endocrinologists is their recommendation on the use of apo B or LDL particle number measurements in order to “achieve effective LDL-C lowering, provide screening recommendations for persons of different ages, and identify special issues for pediatric patients.”
Need to harmonize lipid guidelines
In spite of growing enthusiasm about apolipoproteins, some endocrinologists have said there first needs to be more harmony in lipid guidelines. It is no secret that lipid guidelines have critical differences, including recommended lipoprotein levels for risk assessment, CVD risk estimation methodologies and the need for a treatment target or the use of drugs other than statins.
Though LDL-C remains a primary target in most guidelines, the International Atherosclerosis Society (ISA) favours non-HDL-C for dyslipidemia management, as does the AACE in certain conditions. Non-HDL-C is also considered to have higher predictive capability than LDL-C in a wide variety of clinical situations, and be more practical since it can be performed in a non-fasting state.
Yet another source of much debate concerns differences in approach to CVD risk assessment. Time frames for risk vary from 10-years to life time. On their part, the American College of Cardiologists (ACC) and American Heart Association (AHA) recommend measuring 30-year risk in patients aged 20–59.
CVD risk is defined as the risk of both mortality and morbidity in most guidelines. However, the joint (and revised) EAS/ESC guidelines mentioned above calculate fatal CVD risk only. Many guidelines calculate 10-year risk of CVD. However, ISA recommends measuring the lifetime risk.
Physicians ‘bewildered’
A recent issue of ‘European Endocrinology’ poses some candid questions: Today, “physicians are bewildered by a multitude of guidelines written by different professional societies, which have more diversities than commonalities.” The author calls for “organizing a working group in dyslipidemia management and integrating existing guidelines into a general consensus document.” However, he concludes, “owing to the number of controversial areas, this is not likely to occur soon.”
Healthcare portal Medscape puts the ball back in the clinician’s court – in some senses, restating the obvious. Lipid guidelines do not “override the individual responsibility of health professionals to make appropriate decisions in the circumstances of the individual patients, in consultation with that patient, and, where appropriate and necessary, the patient’s guardian or carer”.