LKM Antibodies: skilled pattern recognition
The detection of liver/kidney/microsomal antibodies (LKM) is one of the most common analytical procedures performed in the autoimmunity laboratory. Several techniques can be currently adopted that allow the detection of LKM in patient serum, such as ELISA, line immunoassay or indirect immunofluorescence. Far from being outdated, indirect immunofluorescence is the major method used for the screening of autoantibodies in autoimmune disease diagnosis. But LKM antibodies detection is one of these tests that require skilled laboratory technicians for an accurate pattern identification. This article gives a few tips that can be helpful for that purpose.
Autoantibody
The detection of antibodies against microsomal antigens from liver and kidney, LKM (liver/kidney/microsomal), is an aid for the diagnosis of type II autoimmune hepatitis (Type II AIH). LKM antibodies belong mainly to the IgG isotype, and three different kinds can be distinguished: LKM-1 antibodies, considered as biomarkers of type II AIH; LKM-2 antibodies, which are present in cases of tienilic acid-induced hepatitis; and LKM-3 antibodies, found in some patients with chronic hepatitis D. LKM-1 antibodies can also be detected in patients of type I autoimmune hepatitis that show negative titres for antinuclear antibodies [1].
Target antigen
Cytochrom P450 II D6, the molecular target for LKM antibodies¸ is a 50kDA protein found in the cytoplasm of all hepatocytes and renal proximal tubular cells. This protein belongs to the microsomal enzymes family, localized in the endoplasmic reticulum membrane [2].
There are two important families of endoplasmic reticulum enzymes, the cytochroms and the UDP-glucuronosyl transferases (UGT). Corresponding to the characteristics of the antibodies directed to those enzymes are a certain number of related specifities (table 1).
Clinical significance
Two distinct subtypes of autoimmune hepatitis, type I and type II autoimmune hepatitis, can be discriminated with the aid of the autoimmune serology: antinuclear (ANA) and anti-smooth muscle antibodies (ASMA) lead to the diagnosis of type I AIH, whereas LKM-1 antibodies assist in the diagnosis of type II AIH. The differing serological reactivities for the two types (ANA, ASMA versus LKM-1) are mutually exclusive, although in rare exceptions with ‘double positive’ serology, the clinical manifestations resemble those of type II AIH. Thus, LKM-1 antibodies are considered as biomarkers of type II AIH [4].
The disease usually starts in childhood and it often shows a severe progression, affecting more frequently women, like most autoimmune diseases. In the U.S.A., LKM-1 antibodies are common in pediatric patients and rare in adults. LKM-1 antibodies can be detected in certain patients with hepatitis C virus infections, not being affected by type II AIH [5].
Screening methods
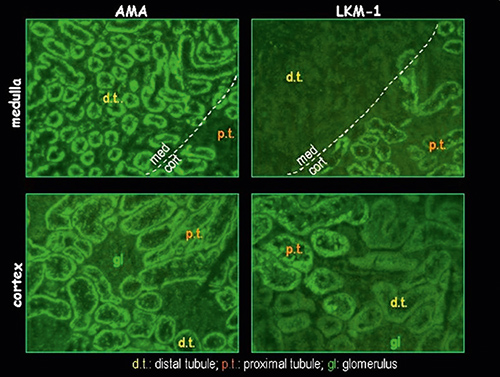
Indirect immunofluorescence on rodent kidney and liver sections is the main technique used to test LKM-1 antibodies in the clinical laboratory. The typical fluorescent pattern observed consists in an intense staining of proximal renal tubules in kidney and intense cytoplasm staining of hepatocytes in liver (Figure 1). Due to the similiarity between the mitochondrial and the LKM-1 patterns, tests manufacturers usually supply slides containing kidney with cortex and medulla, liver and stomach in the same determination well to facilitate the interpretation of LKM antibodies.
A helpful indiction is the negativity of LKM antibodies in the renal medulla, composed only of distal tubules, whereas mitochondrial antibodies stain equally both, proximal and distal renal tubules (Table 2). Among the differential features, mitochondrial antibodies generally show a granular aspect, with glomeruli clearly visible and all tubules stained with certain intensity. On the contrary, LKM-1 antibodies show a non granular staining with glomeruli and distal tubules completely negative.
A part from indirect immunofluorescence on rat kidney and liver sections, ELISA and line immunoassays are techniques commonly used in the clinical laboratory for LKM antibodies determination. The antigen mostly immobilized in this kind of assay is the recombinant cytochrom P450 II D6, used as a capture molecule.
References
1. Homberg JC, et al. Chronic active hepatitis associated with antiliver/kidney microsome antibody type 1: a second type of “autoimmune” hepatitis. Hepatology 1987;7(6):1333-9
2. Manns MP, Griffin KJ, Sullivan KF, Johnson EF. LKM-1 autoantibodies recognize a short linear sequence in P450IID6, a cytochrome P-450 monooxygenase. J Clin Invest 1991;88(4):1370-1378.
3. Strassbourg CP, Manns MP. Autoantibodies and autoantigens in autoimmune hepatitis. In: PD Berk, MP Manns, eds., Seminars in liver disease, 2002, volume 22, number 4: 339-351.
4. Vergani D, Alvarez F, Bianchi FB, Cançado ELR, Mackay IR, Manns MP, Nishioka M, Penner E. Liver autoimmune serology: a consensus statement from the committee for autoimmune serology of the International Autoimmune Hepatitis Group. J Hepatol 2004; 41: 677–683
5. Krawitt,E.L. Autoimmune hepatitis. N Engl J Med. 2006;354(1):54-66.
The author
Petraki Munujos, PhD
BioSystems S.A.
Barcelona
Catalonia (Spain)