Neurocysticercosis: can we trust serology?
Which is the most common parasitic disease of the nervous system, which affection is the leading cause of seizures and acquired epilepsy in the developing world but still preventable? The answer: neurocysticercosis. An orphan disease suffering from the absence of a real ‘gold standard’ diagnosis. Meanwhile, many laboratories perform immunodiagnosis but what is its real value and what can it tell us?
by Dr Jean-François Carod
What is neurocysticercosis?
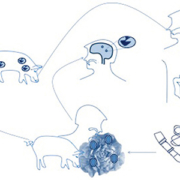
Cysticercosis of the central nervous system (neurocysticercosis) is caused by the larval stage (cysticerci) of the pork tapeworm Taenia solium. When people eat undercooked pork containing viable cysticerci, they develop an intestinal tapeworm infection (Fig. 1). Humans can also become intermediate hosts, however, by directly ingesting T. solium eggs shed in the feces of human carriers of the parasite. These eggs then develop into cysticerci, which migrate mostly into muscle (causing cysticercosis) and into the central nervous system where the cysticerci can cause seizures and many other neurological symptoms, neurocysticercosis (NCC). NCC is a major cause of epilepsy in endemic countries. It is the most important neurological disease of parasitic origin in humans. The pathogenesis is unclear but symptoms seem to correlate with the stage of the cyst. Starting as a viable entity, the cyst then gradually degenerates and become calcified. Seizures seem to appear at the degenerating and calcified stage but treatment is effective on the living cysts. Human cysticercosis is endemic in the Andean area of South America, Brazil, Central America and Mexico; China, the Indian subcontinent, South-East Asia; and Sub-Saharan Africa including Madagascar.
Why do we need to diagnose it?
Diagnosing NCC is required in the event of unexplained encephalitic disorders such as first onset of seizures in countries where NCC is endemic or in patients travelling in countries where NCC is endemic and who may have been at risk of infection (e.g. exposed to NCC risk factors, such as inadequate hand and food hygiene).
How can it be diagnosed?
The diagnosis of cysticercosis of the central nervous system involves the interpretation of non-specific clinical manifestations, such as seizures, often with characteristic findings on computed tomography (CT) or magnetic resonance imaging (MRI) of the brain, and the use of specific serological tests (Fig. 2). Diagnostic criteria based on objective clinical, imaging, immunological and epidemiological data have been proposed but are not generally used in areas endemic for the disease [1].
Serology is indicated for the diagnosis of T. solium seropositivity. But from a positive serology to the assessment of NCC diagnosis, there is a huge gap. A positive T. solium serology is not predictive for a neurological localization and serology may remain positive years after the end of the infection.
No single test can lead to a definitive diagnosis of NCC. CT-scan or MRI may be performed on the presentation of clinical symptoms that could be attributed to NCC (first onset of seizure, unexplained headache…) for people who were exposed to NCC risk factors. Imaging may show typical ring lesions with or without inflammation and calcification. However, the image is not pathognomonic of NCC unless hooks (scolex) are visible inside the ring. Thus, serology may give the clue if positive. A positive serology (antibody) may be confirmed by Western-blot or electro-immuno transfer blot (EITB), which show the typical bands specific of T. solium glycoproteins. Antigen detection in the blood can also be performed. This test is specific for T. solium and does not require laboratory confirmation. Both antigen and antibody assays can be performed in the cerebrospinal fluid (CSF). The presence of antibody or antigen in the CSF may contribute towards the assessment of the neurological localization of the disease. In developing countries, the regions most affected by T. solium infection, CT-scan and, of course, MRI are unaffordable, if ever available.
What are the current laboratory tools?
The laboratory diagnosis of cysticercosis is basically the immunodiagnostic based firstly on antibody detection with ELISA (enzyme-linked immunosorbent assay) or immunoblot.
The detection of antibodies against T. solium is a common method of infection diagnosis, but presents many limitations as a single cyst carrier may not be easily detected. Commercially available tests include essentially ELISA and Western-blots. Western-blots are the ‘gold standard’ assays for the detection of specific antibodies against T. solium. The reference Western-blot assay remains the one developed at the Centers for Disease Control (CDC), Georgia, USA, by Tsang et al. [2]. It employs a specific fraction of T. solium cysts. Many of the components have been identified and cloned. The test is very specific for exposure and/or disease and to confirm the diagnosis. Both ELISA tests and Western-blot relay on antigens that have varied significantly throughout the years (Fig. 3) [3]. Historically, the first assays used crude soluble extracts, then purified proteins such as lentil lectin glycoproteins (LLGPs) Recent trends, though not yet commercialized, tend to emphasize the use of recombinant proteins. Designing recombinant antigens requires a proteinomic approach (Fig. 4) that is now frequently used in development units. Current studies propose the use of nanobodies for diagnostic purposes. These evolutions increased both the sensitivity and the specificity of the tests.
Another available technique is based on the detection of circulating parasitic antigens using monoclonal antibodies [4]. This test is capable of detecting single cyst carriers and is more specific than available antibody ELISA tests. Its main advantage is its ability to monitor the response to cysticidal therapy.
Understanding the performance assessment of T. solium detection tests
Most commercially available ELISA tests have been evaluated by poor methodology. Assessing that a performance evaluation used the proper method means ensuring that the study used a serum bank of parasitologically-defined sera to assess test sensitivity. Defined cysticercosis sera should ideally include the following sera: two or more viable cysts, single viable cysts, degenerating cysts, calcified cysts.
Each series should be initially tested separately. A parasitologically-defined sera should correspond to the Del Brutto criteria [1]. In the absence of a true ‘gold standard’ for the diagnosis of neurocysticercosis, positive sera (cases) should be taken from patients with (1) absolute diagnosis of NCC, or (2) probable NCC diagnosis.
The test specificity should be carefully evaluated using defined negative and potentially cross-reactive sera. Negative sera (control) should be taken from the same area and if possible from people exposed to the same risk factors as the positive cases, with age and sex correlation. Negative cases are usually taken from blood donors of developed countries. Those people have not been in contact with many parasitic infections and the sensitivity of the test will not be accurate/reliable for use in developing countries. This is why specificity should not only be assessed on negative samples from Western countries but also on other parasitic infections from cysticercosis-free developing countries.
What are the new trends in laboratory tests?
If only immunodiagnostic tools based on antibody or antigen detection are currently commercialized, new approaches have been developed including molecular biology (gene amplification in CSF mostly) (Fig. 5). However, so far none constitutes a ‘gold standard’. Table 1 summarizes the pros and cons of NCC diagnosis tools.
Conclusions and future
A test is reliable and useful if it contributes to a care improvement; that is to say to an appropriate therapy for all the patients. As for NCC; the decision to treat is still subject to controversy. Furthermore, even basic serologies are unaffordable or unavailable in endemic countries, not to mention imaging. The key will be in developing a reliable rapid test able to screen infected patients and correlated to neurological lesions of cysticerci.
References
1. Del Brutto OH. Diagnostic criteria for neurocysticercosis, revisited. Pathog Glob Health 2012; 106(5): 299–304.
2. Tsang VC, Brand JA, Boyer AE. An enzyme-linked immunoelectrotransfer blot assay and glycoprotein antigens for diagnosing human cysticercosis (Taenia solium). J Infec Dis. 1989; 159(1): 50–59.
3. Esquivel-Velázquez M, Ostoa-Saloma P, Morales-Montor J, Hernández-Bello R, Larralde C. Immunodiagnosis of neurocysticercosis: ways to focus on the challenge. J Biomed Biotechnol. 2011; 2011: 516042. Doi:10.1155/2011/516042.
4. Garcia HH, Harrison LJ, Parkhouse RM, Montenegro T, Martinez SM, Tsang VC, Gilman RH. A specific antigen-detection ELISA for the diagnosis of human neurocysticercosis. The Cysticercosis Working Group in Peru. Trans R Soc Trop Med Hyg. 1998; 92(4): 411–414.
The author
Jean-François Carod Pharm D, MSc
Laboratoire de Biologie Médicale, GCS de l’ARC Jurassien, Centre Hospitalier Louis Jaillon, 2 Montée de l’hôpital, 39200 Saint-Claude, France.
E-mail: jean-francois.carod@ch-stclaude.fr