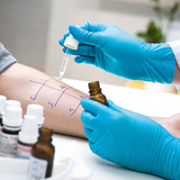
The challenge of food allergies
The threat of allergies, which affect about one in five people in the US and Europe is emerging as a major public health challenge. The problem is also fast becoming severe in the developing world.
Very much an enigma
In spite of these trends, the World Allergy Organisation (WAO) notes that “services for patients with allergic diseases are fragmented and far from ideal,” and that this is true even in the developed world. The key reason is that allergies still remain little understood.
In Europe, for example, the EU Commission acknowledges that the epidemiology of allergies remains “very much an enigma.” In spite of “relatively homogeneous lifestyles” across the region, allergy rates vary from 3.7% among 13-14 year olds in Greece to 32.2% for the same age group in the United Kingdom.
Children hit hardest
As hinted by the EU Commission figures above, the impact of allergies is especially pronounced in a vulnerable demographic, namely children.
Indeed, the Florence, Italy-based European Academy of Allergy and Clinical Immunology (EAACI) reports that “the number of children with allergies has doubled in the last ten years, and visits to A&E have increased seven-fold.” The situation is no different in the US, where a recent study by the Centers for Disease Control and Prevention (CDC) finds allergy to be among the most common medical conditions affecting children aged below 17.
The allergy challenge has been confounded by the fact that its origins now include a bewildering (and growing) range of food products. In Europe, the InformAll Database (developed with funding from the European Union) currently contains information about the “more than 120 foods” reported to be associated with allergy.
The burden of this, once again, is disproportionately high on children. Globally, an estimated 220 to 250 million people could be suffering from food allergy, according to the WAO.
In Britain, the respected National Institute for Clinical Excellence (NICE) zeroes down on food allergy as being “among the most common of the allergic disorders” and “a major pediatric health problem” because of “the potential severity of reactions and a dramatic increase in prevalence over the past recent decades.”
Food allergies a specific challenge
Though the CDC study mentioned above found the biggest challenge for US children to be respiratory allergies, their share – at 17% – has remained constant since the late 1990s. The fastest growth, on the other hand, was shown with skin allergies, up from 7.4% in 1997–1999 to 12.5% in 2009–2011.
In contrast, the prevalence of food allergies in US children is not only smaller than either respiratory or skin allergies, but also showed a slower increase than the latter, from 3.4% to 5.1%.
However, the US figures conceal more than they reveal.
Firstly, managing (or even) identifying food allergies is not straightforward. Unlike respiratory allergies (which have a long-established intervention modus), or skin allergies (which are easier to pinpoint), the diagnosis of food allergies is far more problematic. This is because “nonallergic food reactions, such as food intolerance, are frequently confused” with food allergies.
The allergy continuum
Making things worse is the allergy continuum.
According to a review of two million patient visits in the US (the largest ever of its kind), food allergies in childhood are instrumental in the so-called ‘allergy march’, a medical condition by which there is an escalation in the risk “for the development of additional and more severe allergy-related conditions, including asthma, later in life.”
In other words, tackling food allergies effectively may hold the key to reducing the burden of other allergies in later life.
Profiling allergies: differences between children and adults
Food allergies in children are most commonly caused by eggs, milk, peanuts, tree nuts and wheat; in adults, milk and wheat are excluded as typical allergens, and instead replaced by fish and shellfish.
However, the EU Commission’s observation about the ‘enigma’ of allergies applies to food too. “In continental Europe, the most common food allergies are to fresh fruit and vegetables, whilst in Anglo-Saxon countries hazelnuts, peanuts and walnuts are the most problematic. Allergy to fish and shellfish prevails in Scandinavia and Northern Europe.”
Tracking the severity of allergies
An allergic reaction to food usually occurs quite quickly (in some cases, within minutes of eating a particular food, and in others, 2-3 hours afterwards). Typical symptoms include an abnormal swelling of the tongue, diarrhea, and hives.
In severe cases, the reaction (as with other allergies) is anaphylaxis, which can be life-threatening.
A study by Mayo Clinic covering a period of 10 years (1990 to 2000) found an age-specific rate for anaphylaxis highest in the under-19 year population (at 70 per 100,000 person-years, compared to an overall age- and sex-adjusted rate of just under 50). The Mayo clinic study also found that ingested foods accounted for one-third of all cases (33.2%), significantly ahead of the second- and third-ranked causes: insect stings with 18.5% and medication with 13.7%.
As troubling is the growth in the incidence of anaphylaxis, again in children. Hospital data from New York State shows that hospitalization for anaphylaxis among patients younger than 20 increased more than 4-fold between 1990 and 2006.
Growing costs
The economic impact of food allergy is significant. In the US, children’s food allergies are estimated to cost as much as $24.8 billion per year.
It is also growing. In the UK, hospitalization for food allergies has increased by as much as 500% since 1990.
Food allergies cannot be cured, but they can be managed by dietary control – in other words through avoidance of allergen-inducing foods. However, there is sometimes little room for a learning curve. In certain people, even tiny amounts of a food allergen (for example, 1/44,000 of a peanut kernel) can prompt an allergic reaction.
Currently, aside from avoidance, the standard of care for food allergies remains “ready access to self-injectable epinephrine.”
Both the US National Institutes of Health (NIH) and Britain’s NICE have drawn up recommendations for the diagnosis and management of food allergy. At the European level, the European Academy of Allergy and Clinical Immunology (EAACI) published its first guidelines on the subject in summer 2013.
An ‘allergy epidemic’: the institutional response
However, the challenge of food allergies is likely to continue.
One key gap is an institutional network of qualified specialists, which link in seamlessly into the wider public health system. In 2006, a subcommittee at Britain’s House of Lords concluded that allergy services were insufficient to deal with it and described the growing incidence of allergic conditions as an ‘allergy epidemic’. Their recommendations urged setting up “at least one allergy centre, led by a full time allergy specialist” in each Strategic Health Authority, supported by “a chest physician, dermatologist, ENT specialist, clinical immunologist, gastroenterologist, occupational health practitioner and pediatrician,” and assisted by “specialist nurses and dieticians trained in allergy.”
The House of Lords subcommittee also strongly called for “diagnostic facilities necessary to investigate complex allergies” staffed by personnel who have received “accredited allergy training.” In other words, such a system will only be meaningful if laboratories are harnessed to address the exploding allergy challenge, and provided with sufficient funds for equipment and staff. Until such time, the response will mean little more than using best practices guidelines (from bodies such as the NIH, NICE and the EAACI) to streamline what essentially remains an ad-hoc infrastructure.
The need for support by clinical labs is implicit in the NICE guidelines on food allergies, which stress that “skin prick tests and blood tests are equally cost-effective” and that “blood tests are cost-effective independent of number of individuals tested.” On the other hand, the guidelines also highlight the need for “valid test results” “to reduce incidence of adverse reactions and improve quality of life,” and prevent the (yet unquantified cost of) anxiety and worry, as well as the “avoidance of food that is actually safe to eat.”
The future: no cures in sight, yet
As of now, there is no cure for food allergies.
A seemingly-promising Phase II, randomized, double-blind study on the anti-asthmatic omalizumab against peanut allergy (one of the most dangerous food allergies) was stopped in 2011, with most subjects not reaching the endpoints. The investigators concluded that “no firm conclusions can be drawn” from their effort, but said it deserved “further investigation.”
The omalizumab research actually reached the same deadlock as another similar anti-IgE preparation, HU-9015, in 2003. This study was, ironically, stopped after its sponsors found the prospects for omalizumab to be more promising.
Nevertheless, researchers continue with their efforts, especially with regard to peanut allergy. As of this date, according to a communication from the National Institutes of Health, 14 studies and trials on peanut hypersensitivity alone are recruiting volunteers, one more than for asthma.