From BIOCHIPs to artificial intelligence – defining new horizons in IFA
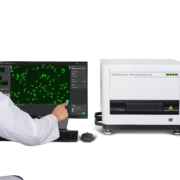
EUROIMMUN has been creating innovative solutions for immunofluorescence diagnostics for over thirty years. CLI talked to Dr. Panagiotis Grypiotis, Head of Product Management Automation at EUROIMMUN, to find out about the company’s milestones and the newest innovations on the market.