Electronic alerts for acute kidney injury: the role of the laboratory
Acute kidney injury is a common and serious complication of many hospital admissions, yet there are often delays in recognizing its development. The laboratory can play a key role in ensuring large increases in serum creatinine do not go unnoticed so that deteriorating patients receive prompt medical attention.
by Nick Flynn
Introduction
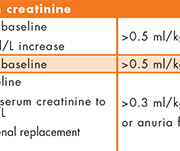
Acute kidney injury (AKI) is a sudden decline in renal function, generally occurring over hours or days. AKI is increasingly recognized as a common healthcare problem associated with poor outcomes such as increased mortality and progression of chronic kidney disease [1], prolonged hospital stay and increased healthcare costs [2]. There is also evidence that management of patients with AKI is sometimes poor: in the UK, a National Confidential Enquiry into Patient Outcomes and Death (NCEPOD) report found severe deficiencies of care in a cohort of patients who died with a primary diagnosis of AKI [3]. For example, there was often a delay in recognizing post-admission AKI. This has prompted some hospitals to implement electronic alerts (e-alerts) to systematically detect and highlight cases of AKI. As current definitions of AKI are based mainly upon changes in serum creatinine, laboratories are well placed to implement these systems (Table 1) [4]. This review will briefly discuss options for e-alerts, some considerations for their implementation, and the evidence base for their use.
AKI e-alerts
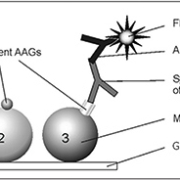
The aim of AKI e-alert systems is to improve the outcomes of patients by facilitating earlier recognition and treatment of AKI. E-alerts may be triggered by a variety of different criteria, ranging from a single threshold creatinine value to full application of AKI diagnostic criteria. This may result in an automated comment being appended to the creatinine result, a phone call, email or text message to the requesting doctor, nephrologist or critical care outreach team, or a combination of the above. The intention is for the alert to prompt medical attention for these high-risk deteriorating patients, with a resulting improvement in patient outcomes (Fig. 1). The most successful e-alert systems are therefore likely to combine the alert with a clinical protocol for AKI management, and should be developed in collaboration with clinical colleagues.
Choosing alert criteria
Although a single threshold creatinine (for example, 300 µmol/L) is the simplest approach, this lacks both sensitivity and specificity for AKI. Creatinine may need to rise significantly before reaching the threshold, so the speed at which AKI is recognized may not be improved. In addition, depending on the population served by the laboratory, a large number of elevated creatinine results are likely to be from patients with stable chronic kidney disease, rather than AKI.
Accuracy can be improved by applying a ‘delta check’ to flag an absolute or percentage increase in creatinine, for example, a 75% increase in creatinine [5]. It is usually within the realms of most modern laboratory information management systems to offer one delta check for creatinine, and it is also sometimes possible to run multiple checks with different criteria. Finally, some systems aim to fully apply current definitions, such as those recommended by KDIGO (Table 1) [4].
Accurately estimating baseline creatinine is difficult
A problem faced both by simple delta checks and e-alerts based on AKI definitions is the difficulty in reliably estimating baseline creatinine. A system employing manual estimation of baseline by clinical biochemists at the Royal Derby Hospital has been shown to have good diagnostic accuracy for detection of AKI with a false negative rate of 0.2% and a false positive rate of 1.7% [6]. However, this approach is limited to normal working hours and many laboratories do not have the resources to replicate this labour intensive system. Instead, automatic surrogate estimation methods are used, such as the lowest, most recent or median creatinine value within a certain timeframe, such as the previous three months. Laboratories should be aware of the limitations of some of these estimation methods; for example, the lowest creatinine result has been shown to be a particularly poor estimate of baseline creatinine that can lead to high rates of potential AKI misclassification [7].
Should every case fulfilling AKI criteria be highlighted?
When choosing criteria for an e-alert system, it may seem sensible to use current definitions for AKI. However, there are arguments against this approach. The KDIGO definition of AKI relies on small changes in serum creatinine based on epidemiological studies which show that even these small increases are associated with an increase in mortality risk in large populations [2]. However, in many cases an increase of 0.3 mg/dl (≥26.5 µmol/L) is within the realms of normal biological variation, particularly amongst patients with chronic kidney disease. As an illustrative example, creatinine increased by between 69% and 129% after the consumption of 300 g of animal protein in healthy volunteers, even with creatinine measurement using a specific enzymatic method [8]. The limitations of the more widely used Jaffe method for serum creatinine are well known amongst laboratory professionals, and any of a wide range of non-creatinine chromogens may cause an increased result in the absence of renal disease. When KDIGO criteria are combined with a poor method of baseline estimation (lowest previous creatinine), the proportion of creatinine results causing an AKI e-alert can approach 10%; this is unlikely to be helpful. Strict application of current AKI definitions could therefore lead to annoyance and unresponsiveness amongst clinicians alerted to minor creatinine elevations, unnecessary interventions, anxiety for patients and families, and diversion of limited healthcare resources to a large and relatively low risk group. It is therefore important for laboratories to consider both local IT and resource capabilities and the relative benefit and harm of different criteria for e-alerts before implementation.
Evidence base
A small number of studies have investigated the effect of AKI e-alerts on clinician behaviour or patient outcomes. For example, a real-time alert of worsening AKI stage through a text message sent to the clinician’s telephone was found to increase the number of early therapeutic interventions in an ICU in Belgium [9]. There was also an increase in the proportion of patients who recovered their renal function within 8 hours after an alert indicating less severe AKI, but not amongst those with more severe AKI. There was no significant effect on renal replacement therapy, ICU length of stay, mortality, maximum creatinine or maximum AKI stage. Importantly, 9 out of 10 AKI alerts were based on urine volume criteria, so the applicability of these findings to creatinine based e-alerts is questionable.
Hospitals that have already implemented AKI e-alerts have noted improved outcomes following their introduction. For example, a hospital-wide e-alert system based on changes in serum creatinine at the Royal Derby Hospital, led to a progressive reduction in 30 day mortality over consecutive 6 month periods (23.7%, 20.8%, 20.8%, 19.5%, chi-square for trend P=0.006) [10]. This improvement in survival was maintained after adjustment for age, co-morbid conditions, severity of AKI, elective/non-elective admission and baseline renal function. However, the e-alert was introduced as part of a range of educational interventions so it is difficult to determine the contribution made by the e-alert component.
The evidence base for AKI e-alerts is therefore not strong, and would benefit from further studies to demonstrate that this approach can lead to measurable improvements in patient outcomes.
Conclusions
E-alerts represent an opportunity for the laboratory to assist in the early detection of acute kidney injury. This could improve the outcomes of patients with this life threatening condition. Aside from AKI, there are undoubtedly many other opportunities for the laboratory to optimize existing resources by helping clinicians to digest the large amount of laboratory data produced on a daily basis, to highlight trends and to ensure that important changes are recognized and acted upon. The laboratory can play a key role to ensure that these systems are implemented, that they are effective in selectively capturing a high risk population, and that evidence is gathered to justify their continued use.
References
1. Coca SG, et al. Long-term risk of mortality and other adverse outcomes after acute kidney injury: a systematic review and meta-analysis. Am J Kidney Dis. 2009; 53(6): 961–973.
2. Chertow GM, et al. Acute kidney injury, mortality, length of stay, and costs in hospitalized patients. J Am Soc Nephrol. 2005; 16: 3365–3370.
3. Stewart J, et al. Adding Insult to Injury: a review of the care of patients who died in hospital with a primary diagnosis of acute kidney injury (acute renal failure). A report by the National Confidential Enquiry into Patient Outcome and Death. London: NCEPOD, 2009. www.ncepod.org.uk/2009report1/Downloads/AKI_report.pdf
4. Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney Int. Suppl. 2012; 2: 1–138.
5. Thomas M, et al. The initial development and assessment of an automatic alert warning of acute kidney injury. Nephrol Dial Transplant 2011; 26: 2161–2168.
6. Selby N, et al. Use of electronic results reporting to diagnose and monitor aki in hospitalized patients. Clin J Am Soc Nephrol. 2012; 7: 533–540.
7. Siew ED, et al. Estimating baseline kidney function in hospitalized patients with impaired kidney function. Clin J Am Soc Nephrol. 2012; 7: 712-719.
8. Butani L, et al. Dietary protein significantly affects the serum creatinine concentration. Kidney Int. 2002; 61: 1907.
9. Colpaert K, et al. Impact of real-time electronic alerting of acute kidney injury on therapeutic intervention and progression of RIFLE class. Crit Care Med. 2012; 40: 1164–1170.
10. Kohle N, et al. Impact of a combined, hospital-wide improvement strategy on the outcomes of patients with acute kidney injury (AKI) [abstract]. Joint Congress of the British Transplantation Society & Renal Association, 2013. Bournemouth. Abstract O30. www.btsra2013.com/
The author
Nick Flynn, Pre-registration clinical scientist
Department of Clinical Biochemistry, University College London Hospitals, London, UK
E-mail: nick.flynn@nhs.net